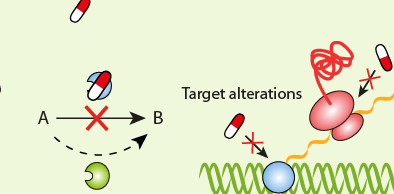
Antimicrobial agents (antibiotics in particular) have helped countless numbers of people worldwide owing to their invaluable role in fighting microbial related infections/diseases; but the effectiveness of these agents and their usefulness for therapy is gradually being tested and deteriorated by the emergence and spread of drug-resistant forms of pathogenic microorganisms that has extended across the community and hospital environments.
The impact and cost of antibiotic resistance on the public health and economy of a nation are enormous. It is therefore imperative that we optimize the use of antibiotics in both our communities and hospitals in order to curtail or abate the development of bacterial resistance which is gradually eroding our therapeutic armamentarium. Due to the selection pressure caused by antibiotic use, a large pool of resistant genes has been created and this resistance places an increased burden on the society in terms of high mortality, morbidity, and cost of treating infections that they cause.
Patients infected with drug resistant organisms are more likely to have ineffective therapy, longer duration of hospital stay, need of treatment with broad spectrum antibiotics that are most toxic and more expensive than their counterparts. All these factors increases the cost of treatment for an individual patient; and on a national or global scale, its effect on the economy can be colossal.
Antibiotic resistance drives up health care cost, thereby increasing the severity of disease and death rates of some infections since not all patients can afford the hospital bill due to the economic situation around. Ineffective treatment due to antimicrobial resistance will eventually culminate to increased human suffering, lost productivity, and often death.
Antimicrobial resistance leads to:
- Increased hospitalization
- Ineffective antibiotics therapy
- Increased cost of treatment
- Morbidity and mortality
- Economic hardship
- Increased severity of infection
- Loss of antimicrobial efficacy of some available drugs
- Spread and emergence of novel drug-resistant microbes
References
Arora D.R (2004). Quality assurance in microbiology. Indian J Med Microbiol, 22:81-86.
Ashutosh Kar (2008). Pharmaceutical Microbiology, 1st edition. New Age International Publishers: New Delhi, India.
Axelsen P.H (2002). Essentials of antimicrobial pharmacology. Humana Press, Totowa, New Jersey, USA. Al-Jasser A.M (2006). Extended – Spectrum Beta – Lactamases (ESBLs): A Global Problem. Kuwait Medical Journal, 38(3):171-185.
Bisht R., Katiyar A., Singh R and Mittal P (2009). Antibiotic Resistance – A Global Issue of Concern. Asian Journal of Pharmaceutical and Clinical Research, 2 (2):34-39.
Joslyn, L. J. (2000). Sterilization by Heat. In S. S. Block (Ed.), Disinfection, Sterilization, and Preservation (5th ed., pp. 695-728). Philadelphia, USA: Lippincott Williams and Wilkins.
Lai P.K and Roy J (2004). Antimicrobial and chemopreventive properties of herbs and spices. Curr. Med. Chem, 11 (11): 1451–1460.
Livermore D.M (2004). The need for new antibiotics. Clinical Microbiology & Infection, 4(10): 1-9.
Mascaretti O.A (2003). Bacteria versus antibacterial agents: An integrated approach. Washington: ASM Press.
Nally J.D (Ed.) (2007). Good manufacturing practices for pharmaceuticals. Sixth edition. Informa Healthcare USA, Inc, New York.
Discover more from Microbiology Class
Subscribe to get the latest posts sent to your email.