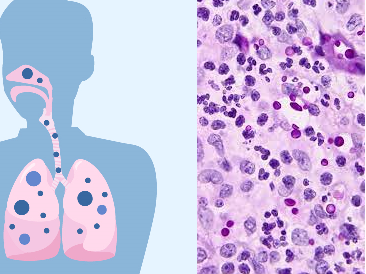
Systemic mycoses are fungal infections that affect deep tissues and organs of the body; and they generally start off as pulmonary infections in affected individuals. They are the most disseminating, deadly and severe forms of mycoses out of all the known fungal mycoses in humans. Systemic mycoses generally involve the internal body organs of humans such as the lungs, heart, liver, bones and kidney; and they also show cutaneous and subcutaneous involvement when the infection is disseminated via the bloodstream. They are mainly caused by dimorphic or diphasic fungi excluding Cryptococcosis neoformans (causative agent of cryptococcosis) which only exist in the yeast form.
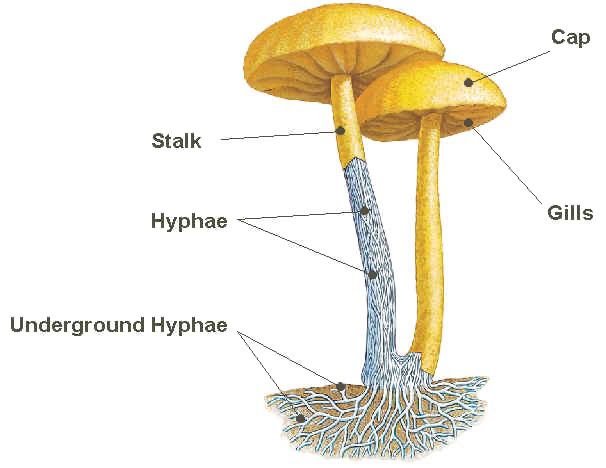
C. neoformans though a causative agent of systemic mycoses also causes opportunistic mycoses in immunocompromised people. Thus, agents of systemic (endemic) mycoses exist in two main forms: the yeast phase and the mould or mycelia phase. Systemic mycoses are usually limited to certain geographic location, and thus they are often referred to as endemic mycoses because they are usually prevalent in certain ecological niches of the world. The viable spores or conidia of causative agents of systemic mycoses grow at ambient temperatures (e.g. 25oC) as moulds in the environment and as yeasts at body temperature (e.g. 37oC) within the human host.
Spores of dimorphic fungi are easily aerosolized and this increases their infectious rate in nature. Systemic mycoses include histoplasmosis (caused by Histoplasma capsulatum), blastomycosis (caused by Blastomyces dermatitidis), coccidioidomycosis (caused by Coccidioides immitis) and paracoccidioidomycosis (caused by Paracoccidioides brasiliensis). Histoplasma, Blastomyces, Coccidioides and Paracoccidioides are found in the fungal division Ascomycota.Brief details of systemic or endemic mycoses are shown in Table 1. Systemic mycosis is initiated following the introduction of fungal spores of dimorphic fungi into the body via inhalation of dust or aerosols containing them.
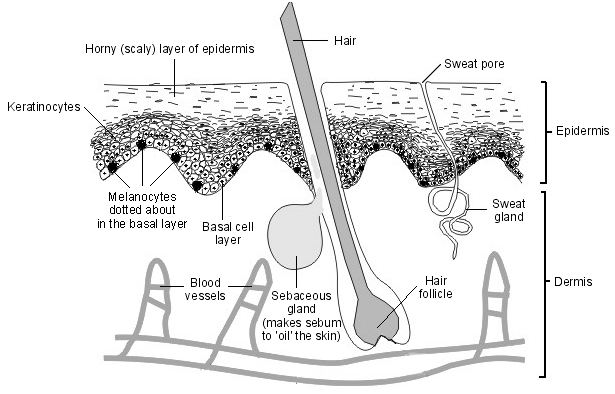
The spores get into the lungs where they grow to cause primary mycosis (e.g. pulmonary disease of the lungs) which is usually self-limiting and asymptomatic in some cases. However, extra-pulmonary mycosis can ensue when the disease becomes chronic and disseminated, affecting other vital organs of the body such as the skin, heart, liver and the kidney. Secondary systemic mycoses usually occur in people with compromised immunity. Systemic mycoses unlike some other fungal infections (e.g. superficial mycoses) are rarely communicable in nature.
Table 1. Synopsis of systemic (endemic) mycoses
| Mycoses | Causative agent | Clinical feature | Site of infection |
| Histoplasmosis | H. capsulatum | Histoplasmosis (or fungus flu) appears as acute and chronic pulmonary disease (e.g. pneumonia) which may be asymptomatic or symptomatic. Granulomatous lesions appear in the lungs; and the liver, spleen and bone marrow may be involved. It mainly involves the reticuloendothelial system (RES); and the lungs, liver, spleen, bone marrow, kidneys, adrenals and intestines are occasionally affected in disseminated cases. Histoplasmosis is common amongst cave explorers and people in contact with the droppings of birds (e.g. poultry birds and bats). Infected persons may experience anorexia, production of purulent and bloody sputum, joint pains and fever. Histoplasmosis is endemic in North America and it occurs in some parts of Central Africa. | Lungs |
| Blastomycosis | B. dermatitidis | Blastomycosis occurs as chronic granulomatous infection of the pulmonary system especially the lungs. Secondary infection occurs when the disease becomes disseminated and affects other organs of the body (e.g. skin). It is similar to histoplasmosis but there is no RES involvement. Symptoms may include chest pain, skin lesions, and fever. The disease also occur in dogs especially in endemic regions but its natural habitat still remains unknown even though it is isolated from the environment. Riverbanks in endemic areas have been attributed as reservoirs of the causative agent of blastomycosis. Blastomycosis is endemic in North America, and it occurs in some parts of Africa. | Lungs and skin |
| Coccidioidomycosis | C. immitis | Coccidioidomycosis or valley fever is a localized self-limiting pulmonary infection of the lungs. Severe pneumonia may occur in some cases; and cutaneous and disseminated forms of infection can also occur especially in immunocompromised individuals. Coccidioidomycosis also involves the subcutaneous tissues, bones and liver. Symptoms may include fever, body rash, meningitis, arthralgia, joint pains and dry cough. Causative agents of coccidioidomycosis are reserved in dry alkaline desert soil. Coccidioidomycosis is endemic in North, South and Central America. | Lungs |
| Paracoccidioidomycosis | P. brasiliensis | Paracoccidioidomycosis or South American blastomycosis is a chronic granulomatous pulmonary disease that may be progressive or disseminated in nature. Mucocutaneous and cutaneous ulcers may ensue; and there is RES and regional lymph node involvement. The natural habitat of the causative agent still remains unknown but its ecological niche has been associated with soil and some animals such as armadillos. It is endemic in Brazil and some parts of Central and Southern America. | Lungs, skin, lymph nodes and mucous membranes of the mouth & nose |
| Cryptococcosis | C. neoformans | Cryptococcosis is an asymptomatic pulmonary disease which usually resolves spontaneously. Chronic and insidious meningitis may also occur in humans due to CNS involvement. Symptoms may include seizures and meningitis, fever, stiffness of the neck, occasional skin lesions and headache. The causative agent is reserved in the soil especially those heavily contaminated with dried bird droppings (e.g. pigeons). Human infections which are most common amongst HIV/AIDS patients and other immunocompromised individuals begin after the inhalation of C. neoformans spores but the organism causes no infection or disease in birds (which serves as its natural reservoir). | Lungs and meninges |
Agents of systemic (endemic mycoses) are ubiquitously found in the soil from where their viable spores or conidia become aerosolized to cause human infection after inhalation. However, an intact and strong immunity is vital to preventing systemic mycosis in humans, but the disease is mostly common amongst immunocompromised individuals and in people with other predisposing health conditions.
References
Anaissie E.J, McGinnis M.R, Pfaller M.A (2009). Clinical Mycology. 2nd ed. Philadelphia, PA: Churchill Livingstone Elsevier. London.
Beck R.W (2000). A chronology of microbiology in historical context. Washington, D.C.: ASM Press.
Black, J.G. (2008). Microbiology: Principles and Explorations (7th ed.). Hoboken, NJ: J. Wiley & Sons.
Brooks G.F., Butel J.S and Morse S.A (2004). Medical Microbiology, 23rd edition. McGraw Hill Publishers. USA.
Brown G.D and Netea M.G (2007). Immunology of Fungal Infections. Springer Publishers, Netherlands.
Calderone R.A and Cihlar R.L (eds). Fungal Pathogenesis: Principles and Clinical Applications. New York: Marcel Dekker; 2002.
Chakrabarti A and Slavin M.A (2011). Endemic fungal infection in the Asia-Pacific region. Med Mycol, 9:337-344.
Champoux J.J, Neidhardt F.C, Drew W.L and Plorde J.J (2004). Sherris Medical Microbiology: An Introduction to Infectious Diseases. 4th edition. McGraw Hill Companies Inc, USA.
Chemotherapy of microbial diseases. In: Chabner B.A, Brunton L.L, Knollman B.C, eds. Goodman and Gilman’s The Pharmacological Basis of Therapeutics. 12th ed. New York, McGraw-Hill; 2011.
Chung K.T, Stevens Jr., S.E and Ferris D.H (1995). A chronology of events and pioneers of microbiology. SIM News, 45(1):3–13.
Germain G. St. and Summerbell R (2010). Identifying Fungi. Second edition. Star Pub Co.
Ghannoum MA, Rice LB (1999). Antifungal agents: Mode of action, mechanisms of resistance, and correlation of these mechanisms with bacterial resistance. Clin Microbiol Rev, 12:501–517.
Gillespie S.H and Bamford K.B (2012). Medical Microbiology and Infection at a glance. 4th edition. Wiley-Blackwell Publishers, UK.
Larone D.H (2011). Medically Important Fungi: A Guide to Identification. Fifth edition. American Society of Microbiology Press, USA.
Levinson W (2010). Review of Medical Microbiology and Immunology. Twelfth edition. The McGraw-Hill Companies, USA.
Madigan M.T., Martinko J.M., Dunlap P.V and Clark D.P (2009). Brock Biology of Microorganisms, 12th edition. Pearson Benjamin Cummings Inc, USA.
Mahon C. R, Lehman D.C and Manuselis G (2011). Textbook of Diagnostic Microbiology. Fourth edition. Saunders Publishers, USA.
Discover more from Microbiology Class
Subscribe to get the latest posts sent to your email.